Physician Fee Schedule 2022: What Providers Need to Know
Each year, the Medicare program updates and publishes final rules governing reimbursement for the Part B fee schedule (typically referred to as the “Physician Fee Schedule”) which becomes effective on January 1st of the following year.
The final rule for FY 2022 was published at the Federal Register on November 19, 2021 and because of previous legislation expiring, the Conversion Factor (part of a complex formula) was set to decrease by 3.73% which would then lead to declining reimbursements overall. Like previous years, Congress “acted,” and the President signed into law on December 10, 2021 the “Protecting Medicare and American Farmers Sequester Cuts Act.” In the end this has resulted in:
-
Most specialties reimbursement will remain flat in 2022. Most specialties will receive increases/decreases between -1% and 1%
-
Other than 5% reductions to both Interventional Radiology and Vascular Surgery.
-
-
The following cuts associated with Sequestration will be minimized (legislation from several years ago) and will require similar legislation next year to avoid future cuts (Sequestration has had the impact of reducing the Medicare fee schedule by about 1.6%-- this reduction will be reduced in 2022):
-
Relief from 2% Medicare Sequester by not beginning it until April 1, 2022 and then reducing it to 1% until June 30, 2022.
-
Halting Statutory PAYGO Sequester for 2022 by adding it to the 2023 scorecard. While this does not remove it completely, Congress will need to take action in late 2022 to eliminate these cuts.
-
Snapshot of Related Highlights
Related highlights pertaining to additional updates include:
CALCULATION UPDATES TO CMS’ FORMULA
CMS utilizes a formula to derive the annual physician fee schedules and the relative value units for work (w), practice expense (pe) and malpractice (mp) have been updated. For this change to meet its regulatory challenge to be revenue neutral, CMS had reduced the “Conversion Factor (CF)” significantly. This reduction was offset by the President signing the “Protecting Medicare and American Farmers from Sequester Cuts Act” on December 10, 2021.
-
Based on RVU changes alone, the majority of specialties are either seeing no overall change or a 1% increase or decrease. However, Interventional Radiology and Vascular Surgery are both seeing a drastic decrease this year of approximately 5%. We have included a summary by specialty later within this report.
EVALUATION AND MANAGEMENT (E/M), CRITICAL CARE AND TEACHING PHYSICIAN UPDATES
In the 2022 Final Rule, CMS made several refinements to the current policies for split (or shared) E/M visits, critical care services, and services furnished by teaching physicians involving residents.
-
These refinements reflect the changing dynamics of medicine with the increasing use of Non-Physician Providers (NPPs), use of Critical Care Services, and clarification of Teaching Physician Services to guard against the possibility of inappropriate coding.
MEDICARE TELEHEALTH
CMS continues to evaluate Telehealth Services and in the 2022 Final Rule, extended through 2023 the additions to the Medicare telehealth services list added temporarily due to the Covid 19 PHE. These services were set to be removed; however, CMS wants the additional time to review data and input to decide on whether these services should be made a permanent part of the Medicare Telehealth List.
-
Telehealth services have been around for several years but with the Covid pandemic driving a dramatic increase in these services, it appears that these services are here to stay. Providers had to quickly ramp up their ability to provide these services during the pandemic and with that ability now in place, it is likely patients will continue to want/need access to care remotely going forward.
QUALITY PAYMENT PROGRAM (QPP)
There are big changes to the MIPS scoring for 2022 performance year. The minimum threshold to avoid penalty and the exceptional performance threshold will increase significantly. New changes introduced in 2022 are the MIPS value pathways (MVPs) and APM Performance Pathway (APP). These are revisions to the existing MIPS program that will support moving towards a greater value of care and create leverage for providers in the program. There will be specialty aligned quality and cost measures to support more meaningful participation.
Calculation Updates
Conversion Factor (CF): While there’s been several moving pieces/legislations, in the end, the 2022 Conversion factor is going from $34.8931 to $34.6062, resulting in a change of -0.82%.
As a result of revisions to certain service’s RVUs, the following exhibit has been prepared by CMS and reflects their estimates to the impact of the various specialties using their own claims data:
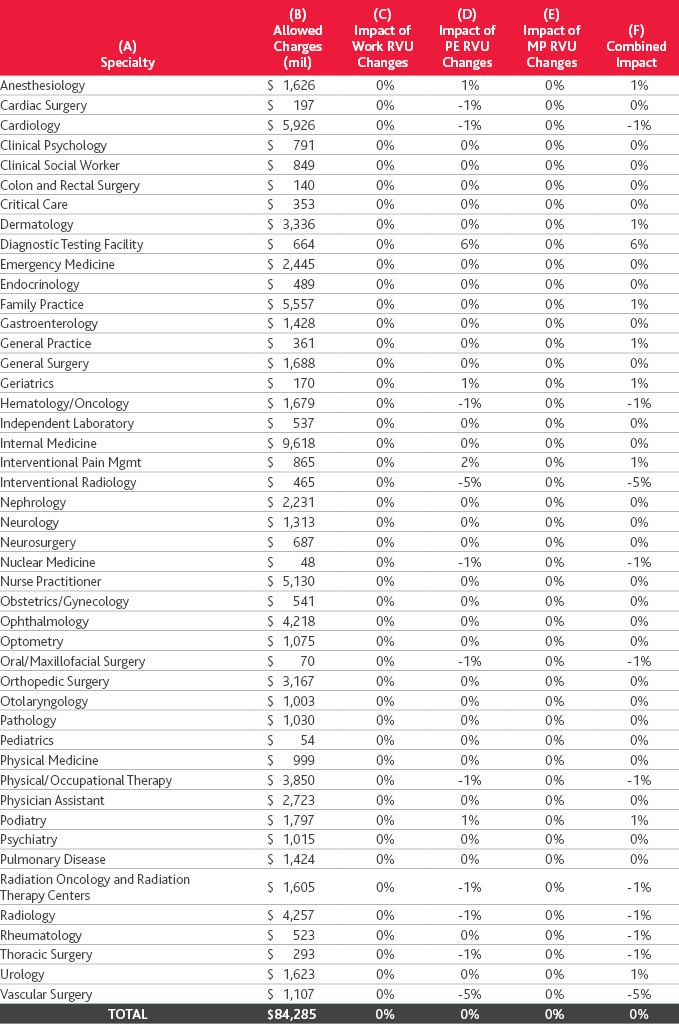
Below is a listing of select services along with a comparison of 2021 vs. 2022 calculations based on RVU and conversion factor changes. These services reflect some of the most significant services for select specialties. The calculations below do not take into consideration the specific geographic practice cost index (GPCI) for any one area.
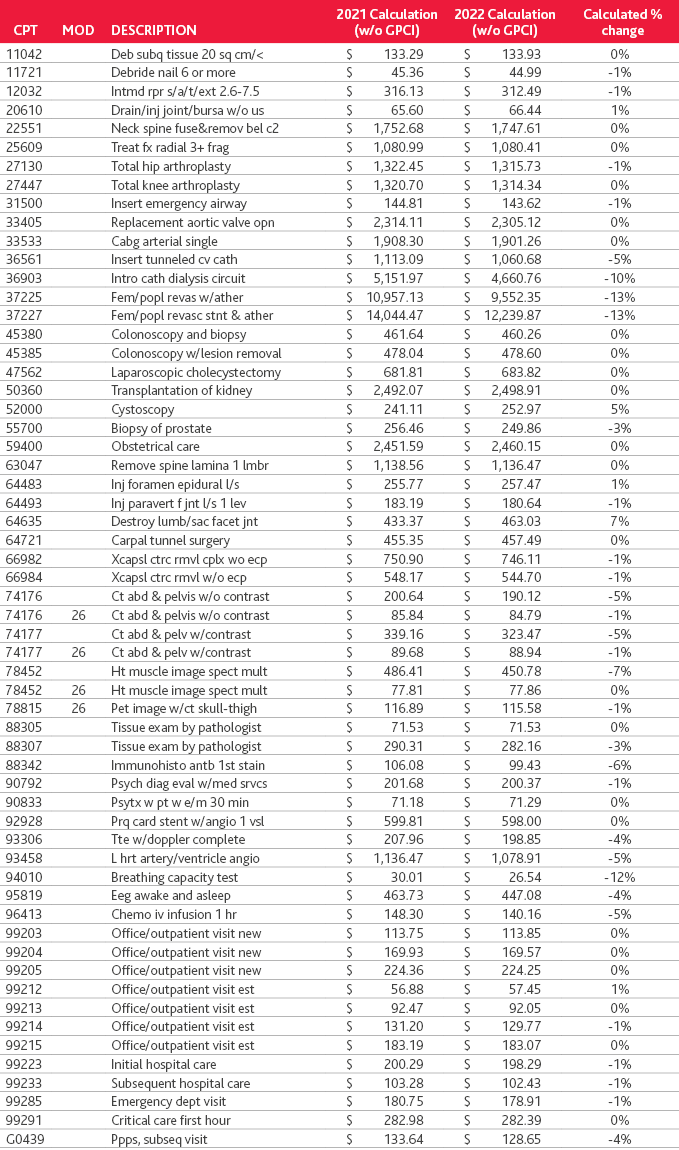
Evaluation and Management (E/M), Critical Care and Teaching Physician Updates
CMS has also clarified and refined some policies that were reflected in certain manual provisions that were recently withdrawn. Specifically, they made several refinements to the current policies for split (or shared) E/M visits, critical care services, and services furnished by teaching physicians involving residents.
Split (or shared) E/M visits –CMS has defined split (or shared) E/M visits as E/M visits provided in the facility setting by a physician and an NPP in the same group. The visit is billed by the physician or practitioner who provides the substantive portion of the visit. These visits can include new as well as established patients, initial and subsequent visits, as well as prolonged services. A modifier will be required on the claim as well as documentation on the medical record of the two people providing the services, with the person providing the “substantive” portion signing and dating the medical record. By 2023, the substantive portion of the visit will be defined as more than half of the total time spent.
Critical Care Services – CMS has refined/established the following guidelines:
-
When medically necessary, critical care services can be furnished concurrently to the same patient on the same day by more than one practitioner representing more than one specialty, and critical care services can be furnished as split (or shared) visits.
-
Critical care services may be paid on the same day as other E/M visits by the same practitioner or another practitioner in the same group of the same specialty, if the practitioner documents that the E/M visit was provided prior to the critical care service at a time when the patient did not require critical care, the visit was medically necessary, and the services are separate and distinct, with no duplicative elements from the critical care service provided later in the day. Practitioners must report modifier -25 on the claim when reporting these critical care services.
-
Critical care services may be paid separately in addition to a procedure with a global surgical period if the critical care is unrelated to the surgical procedure. Preoperative and/or postoperative critical care may be paid in addition to the procedure if the patient is critically ill (meets the definition of critical care) and requires the full attention of the physician, and the critical care is above and beyond and unrelated to the specific anatomic injury or general surgical procedure performed (e.g., trauma, burn cases). CMS is creating a new modifier for use on such claims
Teaching Physician Services – CMS has clarified when time is used to select the office/outpatient E/M visit level, only the time spent by the teaching physician in qualifying activities, including time that the teaching physician was present with the resident performing those activities, can be included for purposes of visit level selection.
Under the exiting “primary care exception” (in certain teaching hospital primary care centers, the teaching physician can bill for certain services furnished independently by a resident without the physical presence of a teaching physician, but with the teaching physician’s review), time cannot be used to select visit level. Only Medical Decision Making (MDM) may be used to select the E/M visit level. CMS feels this is needed to guard against the possibility of inappropriate coding that reflects residents’ inefficiencies rather than a measure of the total medically necessary time required to furnish the E/M services.
Medicare Telehealth
CMS continues to evaluate Telehealth Services that were added during the COVID-19 Public Health Emergency (PHE). They have finalized in the 2022 Rule extension through 2023 the inclusion on the Medicare telehealth services list of certain services added temporarily to the telehealth services list that would otherwise have been removed from the list as of the later of the end of the COVID-19 PHE or December 31, 2021. This will allow time for CMS to gather data and received input on deciding if these services should be permanently added as well as allow time for any wind down for services that may not become permanent, based on the uncertainty of the timing of the end of the PHE.
Expanding on Section 123 of the Consolidated Appropriations Act of 2021 (CAA):
-
CMS has implemented the CAA statutory addition of home of the beneficiary as a permissible originating site for telehealth services furnished for the purposes of diagnosis, evaluation, or treatment of a mental health disorder.
-
Amended the current definition of interactive telecommunications system for telehealth services to include audio-only communications technology when used for telehealth services for the diagnosis, evaluation, or treatment of mental health disorders (established patients) provided in their homes under certain circumstances.
-
Limiting the use of an audio-only interactive telecommunications system to mental health services furnished by practitioners who have the capability to furnish two-way, audio/video communications, but where the beneficiary is not capable of, or does not consent to, the use of two-way, audio/video technology.
-
Finalized the requirement for the use of a new modifier for services furnished using audio-only communications, which would serve to verify that the practitioner had the capability to provide two-way, audio/video technology, but instead, used audio-only technology due to beneficiary choice or limitations.
Quality Payment Program
There are big changes to the MIPS scoring for 2022 performance year. The minimum threshold will increase to 75 points (up from 60 points in 2021) to avoid the -9% penalty in 2024. The exceptional performance threshold increases to 89 points. As a reminder this is a budget neutral program which means the bonus paid will be funded by the penalties applied. For the last two years there haven’t been many penalties since there have been resources such as the hardship exceptions that helped ease the burden of reporting.
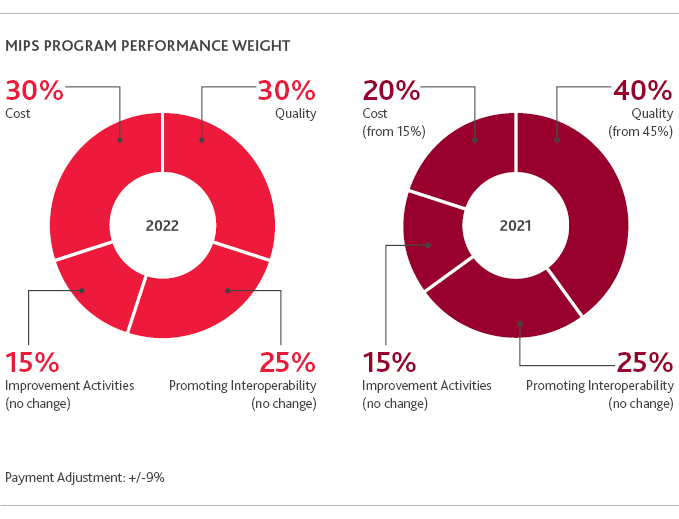
For 2022, Quality and Cost categories will be equally weighted at 30%. While Promoting Interoperability (PI) and Improvement Activities (IA) categories remain the same at 25% and 15%. It has not been released if there will be assistance or exceptions available for groups or clinicians still dealing with the impact of the pandemic in 2022.
New changes introduced in 2022 are the Merit-based Incentive Payment System (MIPS) value pathways (MVPs) and APM Performance Pathway (APP). These are revisions to the existing MIPS program that will support moving towards a greater value of care and create leverage for providers in the program. There will be specialty aligned quality and cost measures to support more meaningful participation. MVPs will combine categories for different specialties or conditions. 2022 will be a testing year and in there will be seven MVPs in 2023 performance year available to join. The MVPs options are advancing Rheumatology patient care, coordinating stroke care to promote prevention and cultivate positive outcomes, advancing care for heart disease, optimizing chronic disease management, adopting best practices, and promoting patient safety within emergency medicine, improving care for lower extremity joint repair and support of positive experiences with anesthesia.
The APP is a single measure set that MIPS APMs can choose to performance in. This was introduced in 2021 and continues to evolve and encourage participation in APMs. This program streamlined quality measures and is optional to report under. Starting in 2025, it will be required for Medicare Shared Savings ACOs to report under APP.
Below is a graphic illustration of the MIPS program for 2022:
Key Takeaways
-
Congress again had to pass legislation to avoid a 3.73% reduction to the Conversion Factor (CF) that would have decreased the fee schedule across all services.
-
The Physician Fee Schedule is essentially flat in 2022 with the exceptions of significant cuts for Interventional Radiology and Vascular Surgery.
-
The green light continues for telehealth services through 2023. CMS will ultimately develop an opinion to the effectiveness of these services, but not for two more years.
-
Beginning with the 2022 performance period, the MIPS Quality and Cost performance categories must be equally weighted at 30%. The industry is still waiting to hear whether assistance or exceptions will be available for groups or clinicians who are still dealing with the impact of the pandemic
It is likely that next year will be more of the same – starting with a statutory reduction in this fee schedule but ultimately with Congress providing a “fix” to maintain access to care issues that could come up.
SHARE